 Multiple Sclerosis and Acupuncture
Multiple Sclerosis and Acupuncture
Are you aware that acupuncture is a great resource for patients who suffer from the Western diagnosis of Multiple Sclerosis (MS)?
Research has shown that Chinese medicine can keep MS patients in remission longer and slow this condition’s progress.[1]
While Chinese medicine cannot cure MS completely, you can feel confident in knowing that it CAN offer considerable help to alleviate symptoms and slow down its progress.
For example, acupuncture can significantly eliminate the feeling of heaviness and tingling in the limbs. And the earlier the treatment is started, the better the results. If treatment is started at the very early stages, the symptoms can be eliminated completely and the progression of the disease halted indefinitely.[2]
The patient should plan on receiving treatment 2-3 times per week for several weeks, and then once a week for a time. Once the patient is stabilized, they should be seen once a month thereafter to keep the disease from progressing.
Let’s consider differences between Western and TCM analysis of MS:
Western Analysis of MS
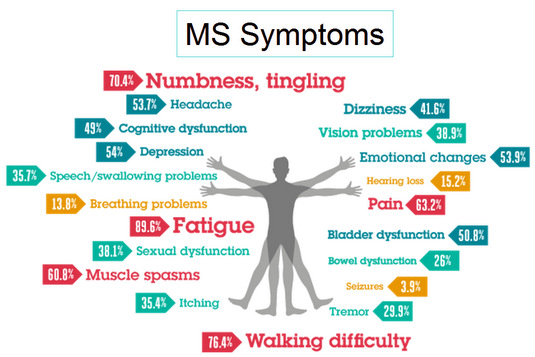
- An autoimmune disorder characterized by patches of demyelination (damage to the protective covering of the neurons) in the brain, optic nerves, and spinal cord. This causes an interruption of signals between the brain and the body.
- Symptoms may include any of the following: numbness of the extremities, trunk or side of the face; weakness of the arms or legs; visual disturbances; problems with bladder control; emotional disturbances; paralysis.
- Shows up without warning, and presents as alternating periods of remission and exacerbation.
- There is no specific treatment.
- As the disease progresses, periods of remission grow shorter and eventually progressive and/or permanent disability occurs.
- Those with MS typically have nutritional deficiencies.
- Intolerances to certain foods are also common.
TCM Analysis of MS
The most common patterns seen for MS patients are Spleen Qi Deficiency, Liver Qi Stagnation, Liver/Kidney Yin Deficiency. These patterns are often complicated by a number of other patterns such as: Damp Heat, Blood Stagnation, Internal Wind (spasms), Kidney Qi Deficiency, and Kidney Yang Deficiency.
Here is a basic explanation and point suggestions for each of the above-mentioned patterns:
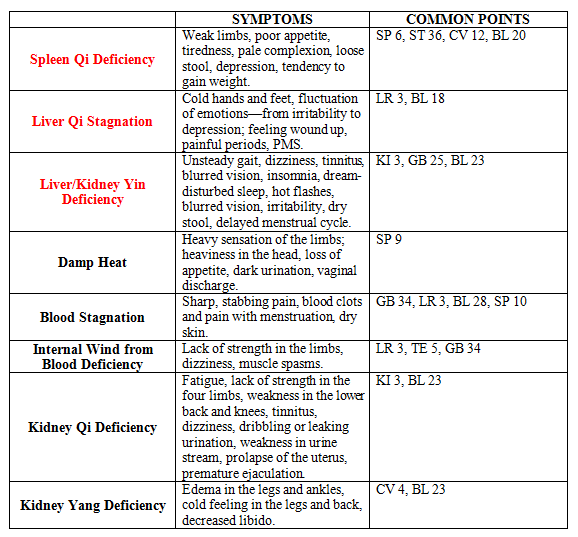
- The first thing to realize is that you ALWAYS have to strengthen the spleen, move liver qi, and tonify liver and kidney yin because this is the base pattern. Do this with every treatment. Then pick out which patterns are showing up for your patient according to their symptoms, and add some of those points to your protocol.
- It is important to teach your patient about a spleen-happy diet, which includes avoidance of foods that are uncooked and adding in foods that help to strengthen the function of the spleen, such as warm root vegetables and soups. A poor diet makes MS symptoms worse.
- Liver qi stagnation exacerbates symptoms! Get your patient on a regular treatment protocol and teach them how important it is to avoid “unnecessary” stress. Help them find ways to move liver qi between treatments. Some suggestions for home treatment remedies include foot rubs with emphasis at Liver 3, going for a walk, or an herbal formula that keeps liver qi moving.
- Help your patients to realize that when they are overtired, their symptoms become worse. MS patients have to learn when to say no to excessive activities. They may also need to be on a formula to supplement their qi.
- Women may experience an exacerbation of their symptoms related to the spleen, liver and wind (bloating, loose stools, irritability, more severe tremors) in association with their menstrual cycle. My female patients who come in once a month for acupuncture do not experience increased premenstrual symptoms.
I’d like to share with you 2 patient examples:
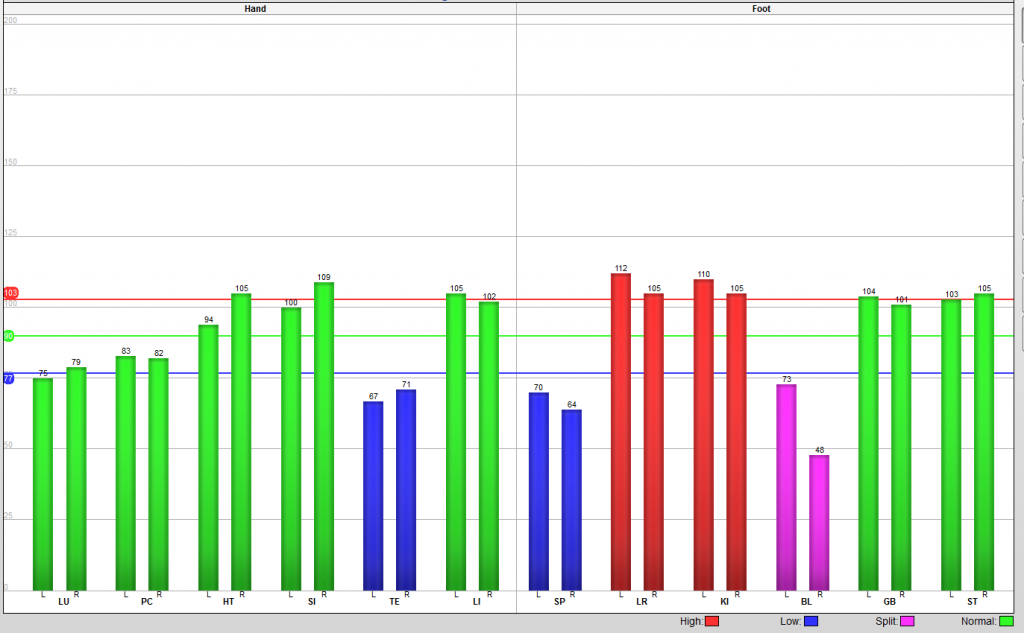
Patient #1: This patient sees me for acupuncture every two weeks to keep her MS in remission. Her TCM pattern diagnosis is: LR/KI Yin Deficiency, SP Qi Deficiency and LR Qi stagnation. She was diagnosed with MS more than 20 years ago.
Patient #2: The next patient was newly diagnosed with MS last year. She does not get acupuncture on a regular basis. Her TCM diagnosis is: LR/Ki Yin Deficiency, SP Qi Deficiency with Damp-Heat in the Middle Jiao, and Blood Stagnation.
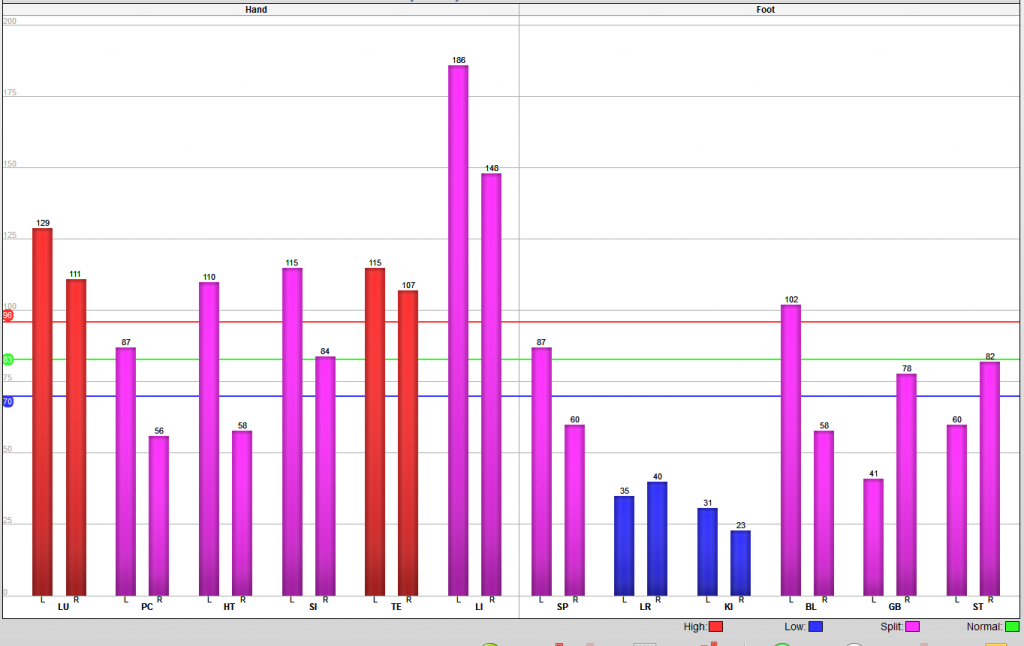
The contrast between the two patients is amazing.
I believe that because patient #1 gets acupuncture on a regular basis, she has been able to keep her MS in remission. She understands the value of continued acupuncture care and comes in for realignment whenever she is feeling stressed–but she does not have particular MS symptoms which she complains about.
Patient #2, on the other hand, only comes in about once a month. She presents with a lot of numbness and tingling down her limbs, a foggy feeling in the brain, stress, depression, and digestive disturbances. She does claim to get relief for some time after each treatment, but I don’t have the opportunity to treat her as often so that she can see continued results.
Education about how Multiple Sclerosis can be treated with Chinese Medicine is a key factor in combating this disease.
Giving the patient scientific evidence of how their condition is improving is VERY beneficial. I have found that they share their graph results with a minimum of 3 family members and friends.
Providing this simple education tool has resulted in more referrals for my practice and better adherence to my treatment recommendations.
If you’re not using the AcuGraph in your practice you are missing ALL of these benefits.
Maybe you have questions and you need answers? I know I did! Click here to view a short video and be sure to catch our next Webinar.
Until then, spread the word that getting treatment early and regularly can keep MS from progressing!
Kimberly Thompson, L.Ac.
Acupuncture Research Analyst
Miridia Technology Inc.
[1] Lu Xi et al., “A Study of the Chinese Medicine Prevention of Relapse of Multiple Sclerosis,” Zhong Yi Za Zhi (Journal of Chinese Medicine), #7, 1995, p. 417-418
[2] Maciocia, “The Practice of Chinese Medicine—The Treatment of Diseases with Acupuncture and Chinese Herbs,” Churchill Livingstone, 1994, p. 706-707



I am a quadruparaeitic since 42 years gradually prograssive. Now I am 69 years with 85% disability is there anything to help me.
I have seen acupuncture change quality of life in a number of patients, often times helping their condition to slow it’s progression. I hope that you are receiving regular acupuncture treatment.
Kimberly
I followed the TCM model and treated diagnostically each time and found a weekly session kept MS under control for a patient in California from November of 2005 to November of 2009. At that time I moved to Wichita and referred them out to another TCM practitioner.
They were quite non-compliant diet-wise and a chain smoker and it still worked. It helped me to realize that non-compliance allows our medicine to shine even more — it radically improved their quality of life. They went from a wheel chair, needing to be moved by helpers to being able to freely move and being able to sense and ward off attacks.
I used TCM acupuncture, tui na (bone setting and rolling), moxa, and qi qong energy.
I was diagnosed with multiple sclerosis 1 month after I turned 50. My Grand-mum was 96 and had it since she was in her 20s. I was on Copaxone, the first year was daily and later I was on 40 mg, 3 times a week. It made a tremendous difference for me. Although the fatigue was what really gets to me. When I do too much, I do start to feel weak.There has been little if any progress in finding a cure or reliable treatment. My multiple sclerosis got significantly worse and unbearable because of my cognitive thinking.. Last year, i started on a natural multiple sclerosis Herbal therapy from Green House Herbal Clinic, i read a lot of positive reviews from patients who used the treatment and i immediately started on it. I had great relief with this herbal treatment. I am doing very much better now, no case of Cognitive thinking or memory Loss,, my multiple sclerosis condition is totally reversed. Visit Green House Herbal Clinic website w ww. greenhouseherbalclinic .com. I am thankful to nature, the medics failed. Share with friends!!
I was diagnosed with multiple sclerosis 1 month after I turned 50. My Grand-mum was 96 and had it since she was in her 20s. I was on Copaxone, the first year was daily and later I was on 40 mg, 3 times a week. It made a tremendous difference for me. Although the fatigue was what really gets to me. When I do too much, I do start to feel weak.There has been little if any progress in finding a cure or reliable treatment. My multiple sclerosis got significantly worse and unbearable because of my cognitive thinking.. Last year, i started on a natural multiple sclerosis Herbal therapy from Green House Herbal Clinic, i read a lot of positive reviews from patients who used the treatment and i immediately started on it. I had great relief with this herbal treatment. I am doing very much better now, no case of Cognitive thinking or memory Loss,, my multiple sclerosis condition is totally reversed.
I have been diagnosed of multiple sclerosis (ms) for 6 years now, i have used so many prescriptions fromm my doctor but never gave me a cure rather controlling the symptoms, my symptoms where ( constipation, depression, difficulty swallowing, difficulty thinking and understanding, flare, headache, heavy legs, numbness of face etc.), my health and life was gradually deteriorating more and more, so i took a glance on the internet and i found (GENERAL HERBAL HEALTH CENTER) a HERBAL MEDICINE HOME that can cure multiple sclerosis (ms), i gave a test to their herbal product because there is no harm in trying, i bought the medicine and it was shipped to my door step and i was very happy so i used the herbal medicine (note: this herbal medicine can be use/taken along with your doctors medical prescription, if you want to) i used this herbal medicine for 9 weeks the results were wonderful, i started getting good result, my symptoms was gradually going away, i started getting healed, i can feel that because i know how i was before i started using the herbal medicine, and in 9 weeks i was cured totally.. thanks to general health center.
.
contact them today via email address: generalhealthcenter1@gmail.com .
After my Multiple Sclerosis diagnosis 2 years ago, i stopped all the Multiple sclerosis medicines prescribed due to severe side effects, and decided to go on natural herbal approach. My primary care provider introduced me to Rich Herbs Foundation and i immediately started on their Multiple Sclerosis herbal formula treatment, this herbal treatment has made a tremendous difference for me. My symptoms including shaking, muscle weakness, fatigue, mood swings, numbness, double vision and urinary retention all disappeared after the 4 months treatment! Their website is ww w. richherbsfoundation. com. Its just amazing!